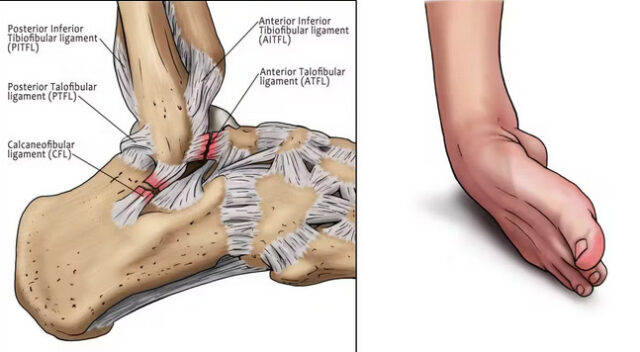
An “ankle strain” (often spoken of alongside ankle sprains) can bench you for days–months depending on severity. Quick recognition, smart acute care, and a rehab plan focused on strength and balance are the difference between a one-off tumble and chronic trouble.
Below I’ve pulled together the essentials, practical steps, red flags, and recent Nigerian players who have experienced ankle problems — all backed by current sports-medicine guidance and news.
Read Also: In Good Shape: Cholera And Sports, Staying Safe – By Dr Kolade Kolapo
Fast facts (need-to-know)
Sprain vs strain: a sprain injures ligaments (bones → bones). a strain injures muscle or tendon (muscle → bone). In everyday sports talk “ankle strain/sprain” is often used interchangeably — but management and prognosis depend on the exact tissue injured.
Most common: lateral (outside) ankle sprains — anterior talofibular ligament most often.
Grading / recovery guide: Grade I (mild) = days–2 weeks; Grade II (partial tear) = ~2–6 weeks; Grade III (complete tear/high-ankle/high severity) = 6+ weeks and sometimes surgery. Individual athletes vary.
What happens on the field / common causes
Rolling, twisting or awkward landings (tackles, jumps, uneven pitches).
Contact collisions or forced inversion (foot turns in).
Fatigue, weak hip/ankle muscles or poor balance increases risk of recurrence.
Immediate on-field steps (first 48–72 hours)
1. Protect: stop play and protect the limb — avoid weight if severe pain.
2. PRICE — Protect, Rest, Ice, Compression, Elevation. (Ice 10–20 min every 1–2 hrs early, compression bandage, elevate above heart when possible). Avoid aggressive heat or massage early if swelling is present.
3. Analgesia: short course of NSAID/acetaminophen as appropriate (follow medical advice).
4. Refer for imaging (X-ray / ultrasound / MRI) if: inability to walk >4 steps, obvious deformity, severe swelling or suspected fracture. (Ottawa ankle rules often used to decide on X-ray.)
Rehab: the stepwise plan that actually works
Modern sports medicine emphasizes criterion-based progression (not just “wait X weeks”) — strength, range of motion, balance, and sport-specific drills must be met before returning. The PAASS framework and several systematic reviews recommend objective testing for return-to-sport.
Typical staged elements:
Phase 1 (days 0–7): control pain & swelling, restore pain-free ROM (gentle ankle circles, alphabet toe movements), continue protected weight bearing as tolerated.
Phase 2 (1–3 weeks): progressive strengthening (theraband dorsiflexion/plantarflexion/inversion/eversion), single-leg balance, neuromuscular drills.
Phase 3 (3–6+ weeks): plyometrics, agility drills, sport-specific cutting/acceleration under progressive load. Objective tests (single-leg hop, strength symmetry, sport drills without pain) should guide final RTP (return to play).
Preventing recurrence (vital — ankle sprains reoccur)
Balance and proprioception training (single-leg balance, wobble board) reduces recurrence.
Strengthen peroneals, tibialis anterior/posterior, hip abductors (weak hip control increases ankle risk).
Use taping or a lace-up brace during high-risk sport or while returning in the first weeks.
Appropriate footwear for surface (firm studs on soft grass; good trainers on turf) and avoid playing on badly uneven pitches when possible. (Contextual tip for Nigerian athletes: poorer pitch quality and travel fatigue increase risk — plan strengthening and recovery accordingly.)
When to see a specialist / red flags
Severe swelling, deformity, numbness, or inability to bear weight.
Persistent instability after conservative rehab (consider specialist assessment for chronic lateral instability).
Recurrent sprains despite rehab — consider imaging and orthopedic/sports med review.
Return-to-play — practical checklist (use with coach/physio)
Athlete should be able to:
Run straight without pain.
Perform sport-specific changes of direction and cutting at game speed without pain or giving way.
Demonstrate strength and hop tests at ≥90% of uninjured side (or meet your team’s objective thresholds).
Have confidence (psychological readiness) — fear of re-injury is common and should be addressed.
Real Nigerian players who have suffered ankle injuries (recent examples & dates)
Victor Osimhen — suffered an ankle sprain during a Nigeria World Cup qualifier (September 2025 reports), with club scans confirming a moderate ligament sprain; he underwent treatment with Galatasaray. This is a high-profile recent example of how quickly a national-team ankle injury can affect club availability.
Alex Iwobi — suffered an ankle ligament injury playing for Everton (January 2023); he missed several weeks while being managed conservatively and scanned to define severity. Shows how club managers rely on imaging and staged rehab.
Samuel Chukwueze — withdrawn from Super Eagles duty in Oct 2024 with an ankle issue and returned to club for assessment/management (example of an international call-up interrupted by ankle problems).
(These are reported examples — ankle problems are extremely common and many Nigerian pros have had them at one time or another; the three above are well-reported, recent occurrences.)
Practical checklist for Nigerian athletes & coaches (quick, actionable)
Warm up 8–12 minutes (dynamic: ankle circles, heel raises, single-leg balance drills).
Include balance/proprioception 10–15 minutes, 3×/week during season.
If rolled ankle on pitch: stop, PRICE, ice, and get assessed same day if you can’t walk 4 steps or pain is severe.
Use a lace-up brace or tape for the first few weeks when returning to training matches.
Keep minimal travel fatigue protocols: sleep, hydration, compression socks when long road/air trips are necessary.
If you’re a player with recurrent sprains ask for structured physiotherapy with functional criteria for return rather than a calendar date.
For enquires/Consultation
Call- Dr kolade kolapo
+234-7032088130